VSP® Orthognathics
Plan with confidence.
Overview
Working in collaboration with 3D Systems, VSP Orthognathics represents a major leap forward in virtual planning of orthognathic surgical procedures. Years of research and patented technology have led to the creation of a protocol that allows for accurate planning and precise clinical transfer via CAD/CAM splint technology.
Features and benefits:
Anatomical design
Case is planned using patient-specific CT data. Allowing for the ability to visualize anatomical landmarks and ensure surgical plan matches patient's anatomy.
Design session
Web-based design session allowing a surgeon direct input on every step of the pre-surgical plan.
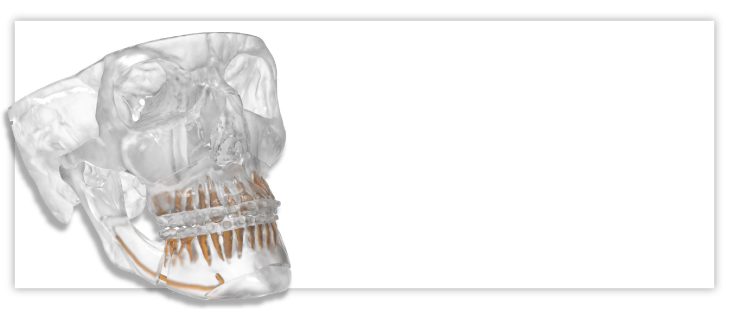
Surgical splints
Surgical splints help transfer the pre-surgical plan into the operating room, helping to ensure accuracy.
Case report
Case report outlines the step-by-step of the of the pre-surgical plan, serving as a reference before surgery and in the operating room.
Clinical evidence
PURPOSE
The purpose of this study was to assess the precision of stereolithographic surgical splints generated by the authors' computer-aided design and manufacturing (CAD/CAM) technique by comparing them with the conventional acrylic splints.
MATERIALS AND METHODS
Seven volunteers were used. A pair of surgical splints, stereolithographic and conventional acrylic splints, was fabricated for each subject. A novel method was developed to quantify the airspace between the teeth and the splint. Conventional acrylic surgical splints served as a control group. The airspaces were recorded by impression materials and sliced cross-sectionally. Corresponding areas of the cross-sectional airspaces between stereolithographic and acrylic splints were measured and compared. Pearson's correlation coefficient and linear regression tests were performed.
RESULTS
Seven pairs of surgical splints were created. The areas of 98 pairs of cross-sectional airspaces were measured. The average difference between the conventional and the STL splints was 0.24 +/- 0.23 mm(2). The correlation coefficient (r) of the airspace areas between the stereolithographic and conventional acrylic splints was 1.00, and the regression coefficient (beta) was 1.03 (P <.01).
CONCLUSIONS
The results indicated that the stereolithographic splints, generated by the authors' CAD/CAM technique, had a high degree of accuracy. The fit of the STL splints was the same as the conventional surgical splints. In the future, traditional plaster dental model surgery will be replaced by computer-assisted surgical planning. The surgical splints will be made in the computer and the treatment plan will be directly transferred to the patient.
PURPOSE
The purpose of this study was to establish clinical feasibility of our 3-dimensional computer-aided surgical simulation (CASS) for complex craniomaxillofacial surgery.
MATERIALS AND METHODS
Five consecutive patients with complex craniomaxillofacial deformities, including hemifacial microsomia, defects after tumor ablation, and deformity after TMJ reconstruction, were used. The patients' surgical interventions were planned by using the authors' CASS planning method. Computed tomography (CT) was initially obtained. The first step of the planning process was to create a composite skull model, which reproduces both the bony structures and the dentition with a high degree of accuracy. The second step was to quantify the deformity. The third step was to simulate the entire surgery in the computer. The maxillary osteotomy was usually completed first, followed by mandibular and chin surgeries. The shape and size of the bone graft, if needed, was also simulated. If the simulated outcomes were not satisfactory, the surgical plan could be modified and simulation could be started over. The final step was to create surgical splints. Using the authors' computer-aided designing/manufacturing techniques, the surgical splints and templates were designed in the computer and fabricated by a stereolithographic apparatus. To minimize the potential risks to the patients, the surgeries were also planned following the current planning methods, and acrylic surgical splints were created as a backup plan.
RESULTS
All 5 patients were successfully planned using our CASS planning method. The computer-generated surgical splints were successfully used on all patients at the time of the surgery. The backup acrylic surgical splints and plans were never used. Six-week postoperative CT scans showed the surgical plans were precisely reproduced in the operating room and the deformities were corrected as planned.
CONCLUSION
The results of this study have shown the clinical feasibility of our CASS planning method. Using our CASS method, we were able to treat patients with significant asymmetries in a single operation that in the past was usually completed in 2 stages. We were also able to simulate different surgical procedures to create the appropriate plan. The computerized surgical plan was then transferred to the patient in the operating room using computer-generated surgical splints.
Abstract
INTRODUCTION:
Patient-specific implants (PSIs) are accurate, efficient
alternatives to traditional plate fixation. They are well-suited for use in
procedures that require the utmost accuracy, stability, and efficiency.
Although PSIs have demonstrated such qualities in craniomaxillofacial
reconstruction, they have so far found limited utilization elsewhere.
CASE PRESENTATION:
We explored the departmental protocol for
Lefort 1 PSI orthognathic surgery at a high-volume, tertiary referral
center. Three cases were selected that matched predetermined criteria,
which included treatment by the same surgical team, concurrent
Lefort 1 osteotomy and bilateral sagittal split osteotomy, Angle’s type
3 malocclusion, lack of interdental osteotomies, and American Society
of Anesthesiologists classification 2 or less without metabolic or
osseous diseases. The operative outcomes from these patients were
then compared to similar cases also meeting the same criteria and
conducted within the same time period.
CONCLUSION:
The use of PSI in Lefort 1 osteotomy is associated with
anatomically sound designs that could contribute to postoperative
stability of the jaws. They also have not shown increased rates of
complications such as infection, dehiscence, or relapse at 6 weeks
postoperatively but may in fact decrease the operative duration. These
findings are consistent with the results gleaned from literature on the
use of PSI in craniomaxillofacial reconstruction.
CMF-WC-64_Rev. None_19003